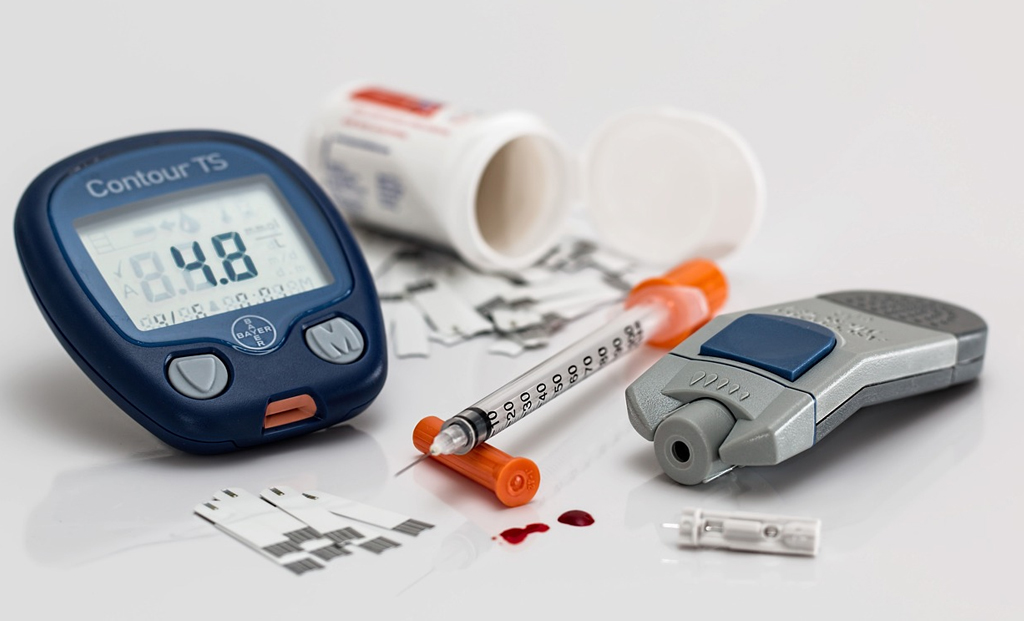
New findings reveal the mechanism through which diabetes hampers the healing process in the eye. A team of researchers, including an Indian-origin scientist, has discovered the factors that contribute to delayed wound healing in the eyes of individuals with diabetes.
While much attention has been given to diabetic eye disease affecting the retina, it is important to note that up to 70 percent of diabetes patients experience issues with the cornea—the transparent, protective outer surface of the eye.
In cases of advanced diabetes, the corneal stem cells lose their functionality, resulting in slower and less complete healing of the cornea following injuries or procedures like cataract surgery and laser treatment for diabetic retinopathy.
The study, published in the esteemed journal Diabetologia, has also identified two cornea-related changes associated with the disease for the first time. Additionally, the researchers have discovered three therapeutic pathways that can reverse these changes and partially restore the cornea’s ability to heal wounds. This groundbreaking discovery may ultimately lead to the development of new treatments for diabetes.
“Current treatments only address symptoms, so there is an urgent need to understand the molecular mechanisms of diabetes-related wound-healing problems,” stated Ruchi Shah, the lead author of the study and a scientist at Cedars-Sinai Medical Center in Los Angeles, USA. She further emphasized the significance of comprehending this novel, epigenetically regulated wound-healing mechanism, as it could potentially pave the way for therapeutic treatments that help patients avoid long-term ocular health complications.
Covid-19 Detection: Scent Dogs Are Rapid And Accurate Alternative To RT-PCR Tests | ALSO READ
Moreover, the research has unveiled the crucial role of Wnt-5a, a secreted signaling protein, in corneal wound healing and the functioning of stem cells—versatile cells capable of differentiating into various types of cells.
“We have discovered that diabetes induces more cellular changes than we were previously aware of,” stated Alexander Ljubimov, the director of the Eye Program at Cedars. He further explained that these discoveries are not related to alterations in gene sequences but rather to specific modifications in DNA that affect gene expression, known as epigenetic alterations. Unlike genetic changes, epigenetic modifications are introduced later in life and are not hardcoded into the genome at birth.
To conduct the study, the team compared corneal cells from six diabetic patients with those from five healthy donors. They observed that in diabetic corneas, the protein produced by the WNT5A gene was suppressed. Additionally, they found an increase in the microRNA that inhibits WNT5A in diabetic samples.
Next, the scientists induced wounds in corneal cells cultured in a laboratory and corneal organ cultures. They tested three interventions aimed at restoring normal Wnt-5a protein expression: direct application of Wnt-5a protein, introduction of a DNA methylation inhibitor initially approved for cancer treatment, and targeting microRNA levels using a novel gene therapy approach involving a nanoscale compound.
7 Indications Of An Unhealthy Gut And The Importance Of Gut Health | ALSO READ
All three therapeutic methods stimulated the production of stem cell markers and improved tissue regeneration, thereby accelerating wound healing in diabetic samples.
“Our objective is to develop topical, sustained-release drugs for corneal wound healing,” said Ljubimov. He expressed optimism that FDA-approved drugs that can be easily applied may represent one of the most promising avenues for effective future therapies.